IPRC Webinar: Documentation Overhaul — Reimagining Family-Friendly Documentation
Tuesday, April 5, 2022
12:00 pm–1:00 pm EDT, 11:00 am–12:00 pm CDT,
10:00 am–11:00 am MDT, 9:00 am–10:00 am PDT
Christine Koterba, PhD, ABBP
Kimberly C. Davis, PhD
Speaker Bios:
Christine Koterba, PhD, ABPP, is a board-certified clinical neuropsychologist in the Department of Psychology and Neuropsychology at Nationwide Children’s Hospital and an Assistant Clinical Professor of Pediatrics at Ohio State University. She is also the attending neuropsychologist on the Inpatient Rehabilitation Unit and the Associate Director for the Pediatric Neuropsychology Internship Track. She serves on the board of the Brain Injury Association of Ohio, is a co-chair of the Education and Advocacy Committee of the International Pediatric Rehabilitation Collaborative, and is a co-chair of the International Neuropsychology Society Brain Injury Special Interest Group. In addition to her work in pediatric rehabilitation and brain injury, she has particular interest on the impact of acquired illnesses with the potential for neurological impact, such as COVID-19 and MIS-C in children. She has published on COVID-related changes to neuropsychology rehabilitation practice and has presented on the impact of the pandemic on children and pediatric neuropsychology.
Kimberly Davis, PhD, is an Assistant Professor in the Baylor College of Medicine (BCM), Department of Pediatrics, Division of Psychology and a Pediatric Neuropsychologist at Texas Children’s Hospital (TCH) in Houston, Texas. Dr. Davis is the Attending Neuropsychologist on the Texas Children’s Inpatient Rehabilitation Unit, where she provides comprehensive assessment, consultation, and family education for children, adolescents, and young adults with recently acquired brain injury. She has also established clinical services and pre-doctoral and postdoctoral training curricula for inpatient neuropsychological consultation and outpatient pediatric cognitive rehabilitation. In addition to her work as a clinician-educator, Dr. Davis leads a number of intraprofessional collaborations aiming to enhance care for youth with acquired brain injury. She is the Vice President of the Pediatric Rehabilitation Neuropsychology Collaborative, serves on the board of the International Neuropsychological Society Brain Injury Special Interest Group, and contributes to subcommittees and work groups through the International Paediatric Brain Injury Society, International Pediatric Rehabilitation Collaborative, and American Congress of Rehabilitation Medicine. She has published and presented on long-term outcomes of pediatric-acquired brain injury and maintains a specific interest in family perceived educational needs throughout the continuum of pediatric brain injury recovery.
Objectives:
At the end of the session, the learner will:
- Discuss 3 challenges to effective communication with families.
- Identify alternative language to use when communicating with families.
- Describe methods to assess caregiver communication preferences.
Audience: This webinar is intended for all members of the rehabilitation team, including medical staff, physical therapists, occupational therapists, speech language pathologists, licensed psychologists, mental health professionals, and other interested professionals.
Level: Intermediate
Certificate of Attendance: Certificates of attendance are available for all attendees. No CEs are provided for this course.
Registration: Registration is complimentary for members of IPRC/RCPA. Registration fee for non-members is $179. Not a member yet? Consider joining today. Multiple registrations per organization are permitted.
Residents Urging Action on Workforce Crisis
In the last month, more than 2,500 residents have contacted the administration and their local state senators and representatives urging them to address the workforce crisis affecting Pennsylvania’s human services sectors.
The outreach has been extraordinary! But we can’t stop now.
The House and Senate will be wrapping up their annual budget hearings over the next few days and turning their attention to crafting the commonwealth’s final spending plan before the end of the fiscal year on June 30.
If you haven’t done so already, please reach out and urge lawmakers to increase funding to support human services professionals so individuals and families in need get the support and care they deserve. Ask your networks to do the same.
Pennsylvania is sitting on billions of federal dollars and state “rainy day” funds that could increase wages to help us attract and retain human service professionals. Yet, even as this workforce crisis worsens, the money remains unspent as the needs of our most vulnerable residents go unmet.
The outpouring of support so far is evidence of how this crisis is affecting individuals and families, as well as the providers and professionals who want to serve them.
But we need to do more…and we need to sustain the effort.
Please VISIT HERE to learn how you can help. Follow us on Facebook and Twitter to stay informed of our progress. Most importantly, TAKE ACTION TODAY. Tell lawmakers to increase funding to address the workforce crisis facing Pennsylvania’s health and human services.
Thank you for your continued support.
Revised Medicare Payment Systems Resource Released
The Centers for Medicare and Medicaid Services (CMS) recently released a revised Medicare Learning Network (MLN) resource, Medicare Payment Systems, to reflect the 2022 regulation changes to payment, quality, and policy for all health settings. These include acute care hospitals, inpatient rehabilitation facilities (IRFs), skilled nursing facilities (SNFs), home health, hospital outpatient, inpatient psychiatric facility, long-term care hospitals (LTCHs), ambulatory surgical centers (ASCs), and durable medical equipment, prosthetics, orthotics & supplies (DMEPOS).
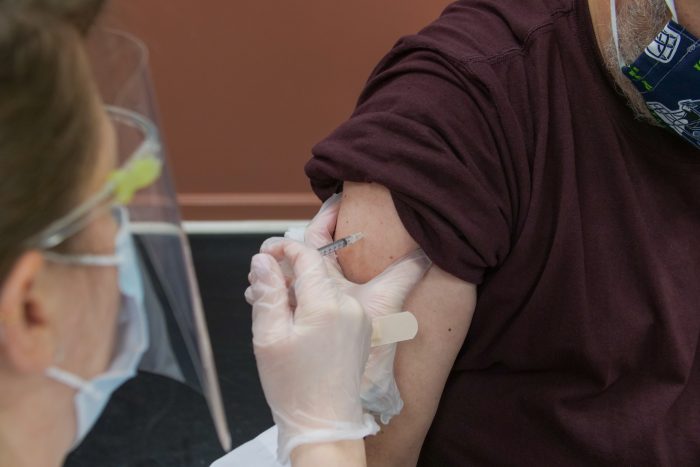
White House Unveils New Plan to Move America Past COVID Crisis

Save the Date: RCPA 2022 Annual Meeting on May 18
ANCOR Capitol Correspondence: The President to Call on Congress for Action During State of the Union Address
COVID-19 Isn’t Going Away, But Health Officials Say Pa. is Ready to Transition to the Next Phase
CMS Redesigns Accountable Care Organization Model
The Centers for Medicare and Medicaid Services (CMS) has announced a redesigned Accountable Care Organization (ACO) model that better reflects the agency’s vision of creating a health system that achieves equitable outcomes through high quality, affordable, person-centered care. The ACO Realizing Equity, Access, and Community Health (REACH) Model, a redesign of the Global and Professional Direct Contracting (GPDC) Model, addresses stakeholder feedback, participant experience, and Administration priorities, including CMS’ commitment to advancing health equity.
In addition to transitioning the GPDC Model to the ACO REACH Model, CMS is canceling the Geographic Direct Contracting Model (also known as the “Geo Model”), effective immediately. The Geographic Direct Contracting Model, which was announced in December 2020, was paused in March 2021 in response to stakeholder concerns. A comparison table of ACO REACH and GDCM is available for additional information.
CMS, through the Innovation Center, is testing new models of health care service delivery and payment to improve the quality of care that people receive, including those in underserved communities. The Innovation Center is making improvements to existing models and launching new models to increase participation in our portfolio, and CMS will be a strong collaborator to health care providers that participate in those models.”
As CMS works to achieve the vision outlined for the next decade of the Innovation Center, CMS wants to work with partners who share its vision and values for improving patient care, guided by three key principles. First, any model that CMS tests within Traditional Medicare must ensure that beneficiaries retain all rights that are afforded to them, including freedom of choice of all Medicare-enrolled providers and suppliers. Second, CMS must have confidence that any model it tests works to promote greater equity in the delivery of high-quality services. Third, CMS expects models to extend their reach into underserved communities to improve access to services and quality outcomes. Models that do not meet these core principles will be redesigned or will not move forward.
REACH ACOs will be responsible for helping all different types of health care providers — including primary and specialty care physicians — work together, so people get the care they need when they need it. In addition, people with Traditional Medicare who receive care through a REACH ACO may have greater access to enhanced benefits, such as telehealth visits, home care after leaving the hospital, and help with co-pays. They can expect the support of the REACH ACO to help them navigate an often complex health system.
The GPDC Model will continue until December 31, 2022, and then will transition to the ACO REACH Model. The first performance year of the redesigned ACO REACH Model will start on January 1, 2023, and the model performance period will run through 2026. CMS is releasing a Request for Applications for provider-led organizations interested in joining the ACO REACH Model. Current participants in the GPDC Model must agree to meet all the ACO REACH Model requirements by January 1, 2023, in order to participate.














