The National Alliance for Direct Support Professionals (NADSP) shared this report:
Direct Support Workforce and COVID-19 National Report: 12-Month Follow-up
READ REPORT
While vaccination rates have improved among professionals supporting people with intellectual and developmental disabilities since the early days of the COVID-19 pandemic, their mental and physical health have declined, a new survey shows.
The Institute on Community Integration, in partnership with the National Alliance for Direct Support Professionals (NADSP), surveyed 2,657 DSPs and frontline supervisors about their experiences supporting people with IDD during the pandemic. The newly released survey report is a 24-month follow-up to an initial report issued in April 2020. Additional surveys were conducted six and twelve months after the initial report. The survey series represents the largest-ever national study of the DSP workforce.
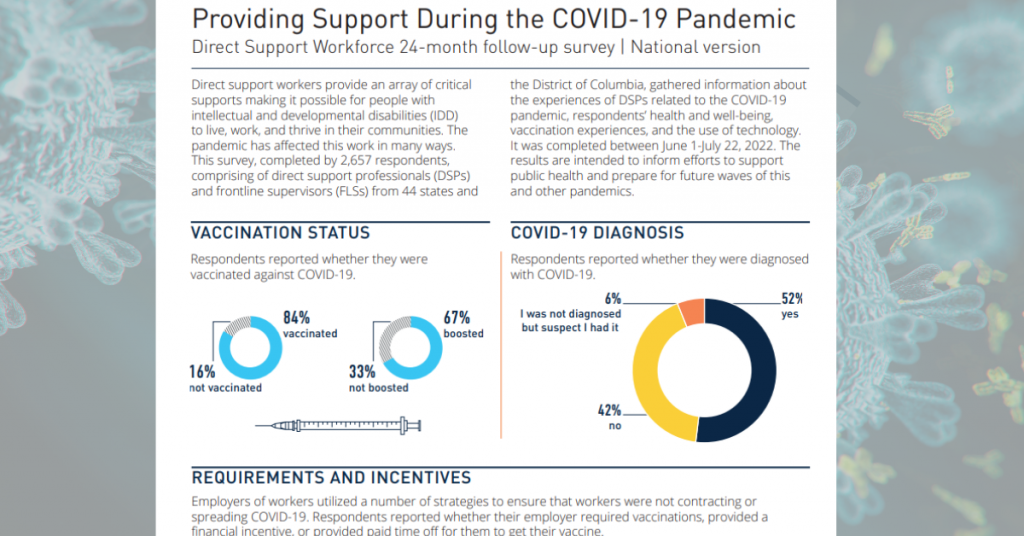
According to the report, 52% percent of DSPs reported being diagnosed with COVID-19, and 6% were not diagnosed but suspected they had it. Among employers, 65% did not require DSPs to be vaccinated.
Sixteen percent of DSPs remain unvaccinated. Of the 84% who are vaccinated, 67% reported having at least one booster shot.
While vaccination rates have improved from the 12-month survey in 2021 (from 72% to 86%), the mental wellbeing of DSPs has declined. Forty percent of DSPs reported experiencing depression, compared with 36% one year ago; 43% had difficulty sleeping, a 13% increase; and 56% reported increased anxiety, a 14% increase. Fifty-nine percent of respondents said they felt pressure to work extra hours.
“Direct support professionals and frontline supervisors have worked as hard as they can,” said Amy Hewitt, ICI director and lead investigator of the study. “This survey shows that their mental health is worsening, and we don’t have the resources to address it. Working this much overtime is not sustainable.”
A national plan to increase the size of the direct support workforce would help to alleviate multiple troubling issues, Hewitt said.
“This workforce has been overlooked and in crisis for years, with high turnover and vacancy rates, low wages, and lack of access to affordable benefits,” she said.
More than half of DSPs receive government-funded assistance, such as housing, energy, food, and healthcare. The pandemic made staffing even more difficult, increasing stress, expectations, and risk on those who remain in their positions.
The 24-month follow-up survey also looked at changes in technology use during the pandemic. Fifty-nine percent of DSPs reported using technology more or a lot more than before the pandemic. Thirty-six percent of the respondents said the use of technology had a somewhat positive impact on their work, and 14% reported it had a very positive impact. Seventeen percent reported a somewhat negative impact and 3% a very negative impact.
Read the full report, a short version, and select state-specific versions here.
Please contact Jerry Smith with questions.

















