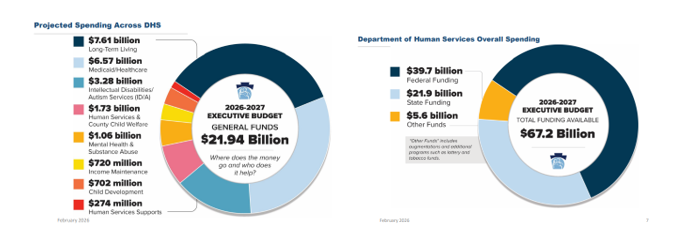
The 2025/26 Budget signed by Governor Josh Shapiro included an additional $13.2 million in state funding for Early Intervention services, with $10 million of this funding specifically targeting provider rates. Last month, the Office of Child Development and Early Learning (OCDEL) released Announcement EI 26-03 and the 2025/26 Fee Schedule, which included a 7% rate increase for Early Intervention services, with some exceptions.
This week, OCDEL announced next steps for a coordinated mass adjustment for processed and paid Early Intervention claims for services delivered in Fiscal Year 2025/2026. The adjustment process will begin the week of March 16, 2026; OCDEL did not give a timeline for completion.
The notice reads:
The Office of Child Development & Early Learning is preparing to perform a Mass Claims Adjustment for all PAID CLAIMS of Early Intervention services that contain a date of service between 7/1/25 – 3/8/26 and were filed on or before 3/8/26. The adjustment process will begin the week of 3/16/26. Due to the high volume of claims, they will be processed in batches. OCDEL is committed to providing updates on the progress of the mass adjustment throughout the week.
Any providers with paid claims that contain a date of service between 7/1/25 – 3/8/26 and were filed on or before 3/8/26 do not need to process their own claims adjustments. When the Mass Claims Adjustment is completed, providers will receive Payment Files and RAs (as applicable) displaying a new ICN beginning with 52. A uniform “billed amount” is being applied to this special Mass Adjustment of $1,000. All claims will correctly “cut-back” to the new Fiscal Year 2025-2026 rates.
Providers are responsible for the following:
- Using the newly published Fiscal Year 2025-2026 Fee Schedule — File NEW claims on or after 3/9/26 that contain a date of service on or after 7/1/25.
- Using the newly published Fiscal Year 2025-2026 Fee Schedule — Adjust claims filed on or after 3/9/26 that contain a date of service on or after 7/1/25 if the OLD fee schedule was used
While it is not recommended that providers submit their own Claims Adjustments for PAID CLAIMS of Early Intervention services that contain a date of service between 7/1/25–3/8/26 and were filed on or before 3/8/26, this will not impact the OCDEL initiated Mass Claims Adjustment.
For OCDEL initiated Mass Claims Adjustments, denied claims will be reported directly from our MMIS provider to OCDEL. In the unlikely event of a Mass Claims Adjustment denial, an OCDEL team member will reach out to the County in which your claims denied to coordinate corrections.
OCDEL would like to remind providers of the timely filling of all claims.
Timely Filing
The regulation at 55 Pa. Cde § 1101.68 (relating to invoicing for services) establishes requirements for submitting claims for services rendered. Early Intervention evaluations, IFSP services and Service Coordination claims are all required to follow this regulation.
There are only a few exceptions that are permitted which are related to PELICAN-EI record issues when there is a change of the child’s MCI or a record change for an adoption. OCDEL is not permitted to allow payment for claims submitted beyond the 180-day regulatory timelines for reasons including but not limited to provider billing errors, billing software issues or personnel vacancies/absences.
Any claims filed after the 180-day filing limit will result in a suspended status. When this happens, an email must be sent immediately to [email protected] with the ICN for the suspended claim and a description for the system reason. If an email regarding the suspended claim(s) is not received, the claim will be automatically denied.
Please forward this message to your contracted providers and direct any questions to your assigned EI Advisor.
OCDEL would like to remind providers of the opportunity to receive claims processing training Gainwell Technologies.
Gainwell Technologies offers PROMISe™ enrollment and billing training for Early Intervention providers. Accessing these training courses is a good opportunity for all Early Intervention providers to be supported in implementing accurate enrollment and billing practices.
PROMISe™ Provider Education & Training:
Webinar recordings are available on the website related to:
- How to Submit 180 Day Electronic Submissions and ACN Electronic Attachments
- How to Submit Revalidations, Reactivations, and Change Request Applications
Provider Portal Training on the topics listed below are also offered on request. Training is conducted via a virtual room (VR) and can be requested via email.
Providers should please include the following information when making a request: 13-digit Provider Number, Provider name, Contact name and phone number:
- Review of PROMISe™ Portal including registration
- Eligibility Verification
- Claim completion review (new, adjustments and voids)
- Claim Inquiry Search
- Enrolled Provider Search
- ERA and EFT Enrollment
- Review of Remittance Advice Statement
- Enrollment Information
- Review of DHS Website including fee schedule, MA regulation, MA Bulletins and Provider Quick Tips
Questions should be directed to the County in which services are contracted.
Visit here for more information on Claims Processing Steps. Contact Cindi Hobbes if you have any questions.











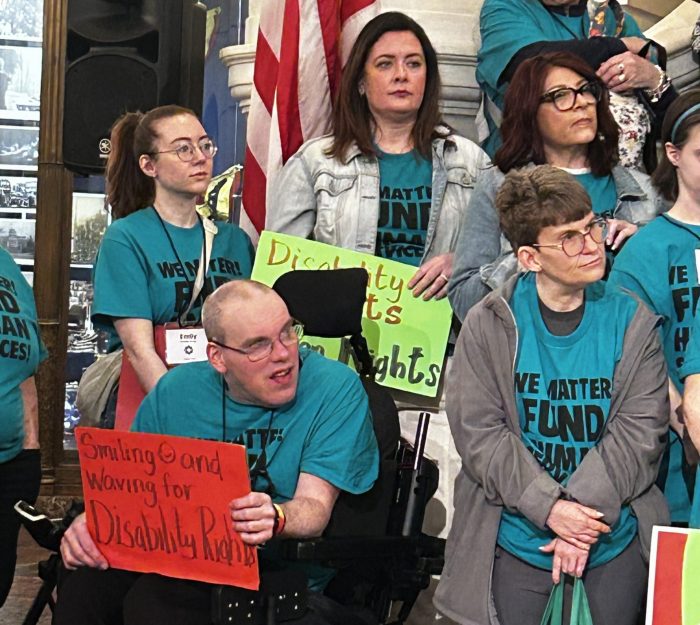
 Richard Edley, President and CEO of RCPA, addressed key points from
Richard Edley, President and CEO of RCPA, addressed key points from 





 RCPA thanks everyone who attended, the legislators who spoke and met with our members, and those who serve our state. We also thank the media outlets who attended, giving more exposure to the issues we face. We will always strive to support you and your communities!
RCPA thanks everyone who attended, the legislators who spoke and met with our members, and those who serve our state. We also thank the media outlets who attended, giving more exposure to the issues we face. We will always strive to support you and your communities!